Milk is a common dietary staple for many people, providing essential nutrients and a sense of comfort. However, for individuals with milk allergy, consuming milk or dairy products can trigger an immune response leading to various symptoms. It is important to understand the signs of milk allergy to ensure prompt diagnosis and appropriate management. ottercovebandb aims to shed light on milk allergy symptoms, causes, diagnosis, and management strategies.
What Is Milk Allergy?
Milk allergy is an adverse immune response to proteins found in milk, primarily cow’s milk. When a person with milk allergy consumes milk or milk-containing products, their immune system mistakenly identifies the proteins as harmful invaders and releases antibodies to fight against them. This immune response leads to a range of symptoms that can vary in severity from mild to life-threatening.
Causes of Milk Allergy
The exact cause of milk allergy is not fully understood, but it is believed to be a result of a combination of genetic and environmental factors. Some individuals may have a genetic predisposition to developing allergies, and exposure to cow’s milk protein at an early age could increase the risk. It is important to note that milk allergy is different from lactose intolerance, which is the inability to digest lactose, the sugar found in milk.

Common Symptoms of Milk Allergy
Milk allergy can manifest with various symptoms that can affect different systems of the body. The symptoms may appear within a few minutes to a few hours after consuming milk or milk products. The common symptoms of milk allergy include:
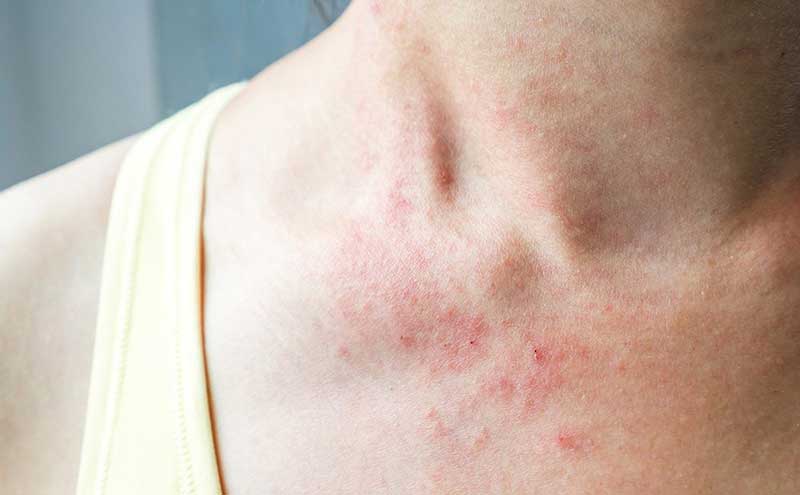
Skin-related symptoms
- Hives (itchy, raised welts on the skin)
- Eczema (itchy, red, and inflamed skin rash)
- Swelling of the lips, face, or throat
Gastrointestinal symptoms
- Nausea, vomiting, or diarrhea
- Abdominal pain or cramping
- Blood in the stool
Respiratory symptoms
- Runny or stuffy nose
- Sneezing
- Coughing
- Wheezing or difficulty breathing
Systemic symptoms
- Anaphylaxis (a severe, potentially life-threatening allergic reaction characterized by difficulty breathing, drop in blood pressure, and loss of consciousness)
It is essential to seek medical attention if anaphylaxis is suspected, as it requires immediate emergency treatment.
Diagnosing Milk Allergy
Diagnosing milk allergy involves a comprehensive evaluation of the individual’s medical history, a physical examination, and allergy testing. The allergist may perform skin prick tests or blood tests to assess the specific IgE antibodies produced in response to milk proteins. In some cases, an oral food challenge may be conducted under medical supervision to confirm the diagnosis.
Managing Milk Allergy
The primary management strategy for milk allergy is complete avoidance of milk and milk products. This requires careful reading of food labels to identify hidden sources of milk protein and adopting alternative dietary choices. Individuals with milk allergy should work closely with healthcare professionals and dietitians to ensure proper nutrition and adequate calcium intake.
Milk Allergy vs. Lactose Intolerance
It is important to differentiate between milk allergy and lactose intolerance, as they have different underlying causes and management approaches. Milk allergy involves an immune response to milk proteins, while lactose intolerance results from an enzyme deficiency that impairs the digestion of lactose. Lactose intolerance primarily leads to gastrointestinal symptoms, such as bloating, gas, and diarrhea, whereas milk allergy can involve a broader range of symptoms.
Potential Complications of Milk Allergy
If milk allergy is not properly managed, it can lead to potential complications, especially in severe cases. Some possible complications include:
- Failure to thrive or poor weight gain in infants
- Nutritional deficiencies, particularly calcium and vitamin D
- Increased risk of other food allergies or allergic conditions
- Emotional and social challenges due to dietary restrictions
Milk Allergy in Infants and Children
Milk allergy is relatively common in infants and young children, affecting around 2-3% of infants. It is one of the most common food allergies in childhood, often outgrown by the age of 3-5 years. Infants with milk allergy may experience symptoms such as colic, reflux, eczema, or gastrointestinal issues. It is crucial for parents and caregivers to be aware of the signs and consult a healthcare professional for proper management.
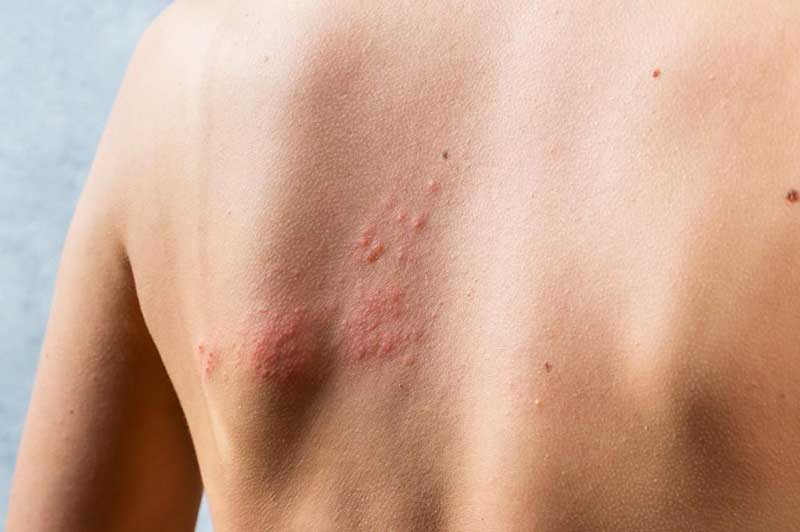
Milk Allergy in Adults
While milk allergy is more prevalent in children, it can also occur in adults. Some individuals may develop milk allergy later in life, even if they had previously tolerated milk without any issues. Adult-onset milk allergy can present with a range of symptoms, including digestive problems, skin reactions, or respiratory issues. Consulting an allergist is essential for accurate diagnosis and appropriate management.
Allergy to Different Types of Milk
Although cow’s milk is the most common trigger for milk allergy, individuals can also be allergic to milk from other animals, such as goat’s milk or sheep’s milk. The proteins in these milks are structurally similar to those in cow’s milk, leading to cross-reactivity in some cases. It is important to identify and avoid all sources of allergenic milk proteins based on individual allergic reactions and medical advice.
Tips for Living with Milk Allergy
Living with milk allergy requires diligence and careful planning to avoid accidental exposure to milk proteins. Here are some tips for individuals with milk allergy:
- Read food labels carefully to identify milk protein sources.
- Be cautious of cross-contamination in food preparation.
- Inform friends, family, and caregivers about the allergy to ensure safe environments.
- Carry an epinephrine auto-injector (such as an EpiPen) in case of severe allergic reactions.
- Seek support from allergists, dietitians, and support groups to manage the condition effectively.
Conclusion
Milk allergy is an immune response triggered by proteins in milk, leading to a wide range of symptoms. It is essential to recognize and understand the signs of milk allergy to ensure timely diagnosis and appropriate management. By avoiding milk and milk products, individuals with milk allergy can lead healthy lives and minimize the risk of complications.
FAQs
Can milk allergy be outgrown?
Yes, many children outgrow milk allergy by the age of 3-5 years.
Are all milk substitutes safe for individuals with milk allergy?
No, some milk substitutes may contain hidden sources of milk proteins. It is important to read labels carefully and consult with a healthcare professional.
Can milk allergy cause asthma symptoms?
Yes, milk allergy can manifest with respiratory symptoms, including wheezing and difficulty breathing.
Is lactose-free milk safe for individuals with milk allergy?
No, lactose-free milk still contains milk proteins and is not suitable for individuals with milk allergy.
Can breastfeeding prevent milk allergy in infants?
While breastfeeding is beneficial for infants, it may not prevent milk allergy. Allergies can develop regardless of breastfeeding status.



